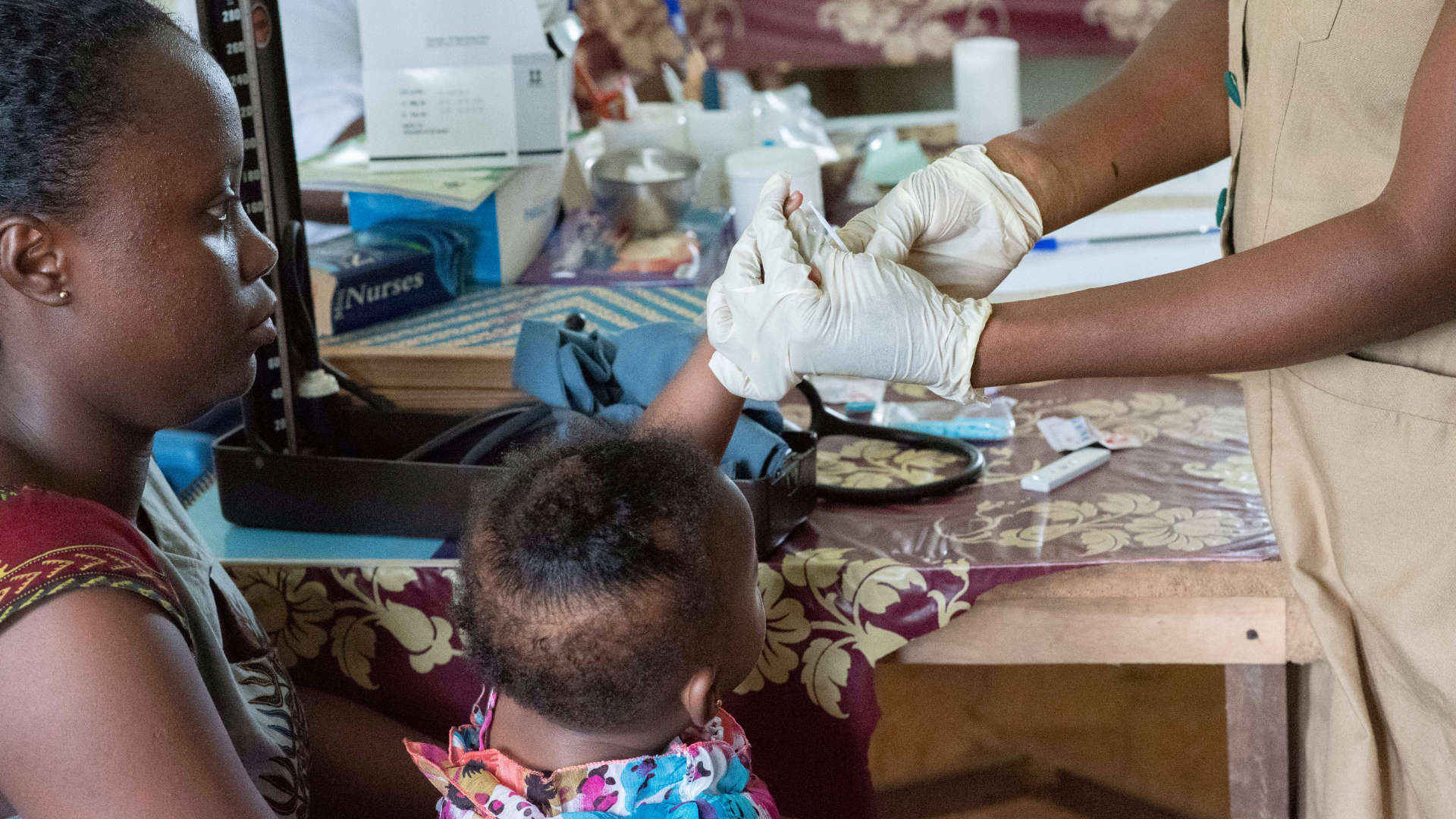
Mr. Hamidu remembers the day – July 20, 2010 – when he was told he was HIV positive. Diagnosed at a public health facility in Kotido District, Uganda, he immediately started on HIV treatment. He receives care and treatment at a military outpost supported by the Department of Defense HIV/AIDS Prevention Program Uganda (DoD Uganda URC Project). Hamidu is one of 2,229 HIV-infected military personnel and family members accessing care at temporary mobile military outposts.
Provision of care at mobile military health outposts has presented challenges with patient retention and treatment follow-up. Since his HIV diagnosis, Hamidu has transferred locations through his military service twice, complicating his access to treatment and care. Other barriers to accessing services have included long and expensive trips to health facilities on poor roads and getting the required military permission to leave the barracks. Also, the process for obtaining monthly drug refills has not been easy.
Thanks to the project-supported military outpost outreach service, Hamidu has been able to receive drug refills and other services at convenient locations, greatly improving access to the treatment and medications he needs.
With support from the DoD Uganda URC Project, military health facilities offering ART across Uganda mapped out military outpost locations in hard-to-reach areas. This differentiated care, tailored to the military population, aligns with the Ministry of Health’s differentiated service delivery model guidelines that seek to address client-related barriers that hinder retention in care.
“I am now at a level of someone who is not sick. I get drugs in time. I just have to adhere to my regimen,” said Hamidu. To ensure timely three-month drug refills, drug delivery has been incorporated into the distribution cycles of other military supplies to the outposts. And mobile outreach clinics are now scheduled once every six months at the outposts to ensure patients receive clinical monitoring whereas in the past, clients had to travel to distant health facilities for monitoring.
Data from February-November 2019 demonstrate that implementing the military-tailored differentiated service delivery model has succeeded in reaching most military personnel on ART who are deployed at outposts. For troops at outposts in select health facilities, retention in care improved from 50% to 90%. Viral load coverage improved from 10% to 62% and suppression rates improved from 64% to 85%. Fifty-five% of the soldiers were transitioned to a new and more effective line of antiretroviral treatment, known as TLD.
In addition, there was an increase in uptake of Isoniazid preventive therapy to reduce the burden of TB among the HIV-positive troops at the outposts: uptake increased from 10% to 38% in 60 hard-to-reach areas served by the military health facilities.
Lastly, stigma for troops living with HIV has been reduced as HIV counseling and treatment now are part of the health services offered at the outposts. “I move with my drugs in the pocket and I take them at noon every day, no matter where I am,” Hamidu said.
Any opinions, findings, and conclusions or recommendations expressed in this material are those of the author(s) and do not necessarily reflect the views of the Defense Health Agency.